"The Mental Health Impact of Burnout and PTSD in Healthcare Workers"
Understanding and Addressing PTSD and Burnout in Healthcare Workers.

The mental Health Impact of Burnout and PTSD on Healthcare Workers
Healthcare workers in the demanding and high-pressure healthcare industry work long hours to provide exceptional patient care, exceeding expectations. Healthcare workers are fully committed to their patients and may be at a higher risk of developing PTSD burnout. This article explores the impact of burnout and PTSD in healthcare workers. It also provides helpful strategies for effectively managing and preventing these conditions.
The Stains of Burnout and PTSD on the Healthcare Industry
Burnout can lead to post-traumatic stress disorder, also known as PTSD. This condition affects a person's mental well-being. Every nurse can potentially experience PTSD. A study in The Journal of Heart and Lung Transplantation found that nurses in intensive care units often have higher levels of post-traumatic stress disorder PTSD).
Emergency healthcare personnel often experience PTSD and burnout in repeated exposure to traumatic work situations. Let's first define PTSD and burnout. Post-Traumatic-Stress-Disorder can be triggered by witnessing patients in critical condition or experiencing the loss of life. Burnout is caused by ongoing workplace stress that hasn't been properly managed.
It has three key dimensions:
- Feelings of energy depletion or exhaustion.
- A growing emotional detachment from work and a sense of negativity or skepticism towards one's profession.
- Reduced professional efficacy and "quiet quitting."
Nurses often experience burnout when caring for sick patients who need help breathing or on critical medications to stay alive. These situations can be life-threatening and contribute to their feelings of burnout. The distinct nature of their work environments contribute to feelings of unhappiness and frustration. Nurses that work in a hospital experience more frequent stressful situations compared to nurses in outpatient settings.
Not all nurses in specialized areas will develop PTSD. Different nurses adapt differently to specific work environments, and factors like workplace stress and personal experiences outside work affect their vulnerability. Healthcare personnel often experience PTSD and burnout due to repeated exposure to traumatic working conditions and experiences.
Some of these symptoms may include:
- Limited resources of hospitals, such as needed PPE that is not available or notably reduced staff.
- Required overtime because there may not be enough staff to take care of patients.
- Healthcare companies are always cutting budgets, including staff and support.
- Disruption of sleep patterns. Healthcare workers are required to work all hours of the day.
- Work-life balance may be upset because of the time spent at the hospital caused by understaffing, required overtime, etc.
Long hours, lack of sleep, and inadequate support can all contribute to burnout symptoms and exacerbate the effects of PTSD. Healthcare workers who suffer from PTSD may become emotionally detached or irritable, which can lead to difficulty interacting with patients or colleagues. They may also struggle with guilt and shame as they cope with the trauma they have experienced during their work.
The Impact of Burnout and PTSD on Healthcare Workers
Let's look at the emotional stress healthcare workers face. High-stress jobs demand personal and organizational steps to handle burnout. Factors like excessive work contribute to burnout syndrome. The physical and mental workload can impact worker performance and well-being. Heavy workloads or poor physical health can lead to conditions like burnout.
Post-traumatic stress disorder related to work is becoming more common among nurses worldwide. Because of this, focusing on improving the well-being of nurses should be paramount. PTSD can cause negative feelings, mental problems, and physical health issues. Nurses with PTSD often start to do worse at work and have problems with things like getting along with others, handling personal matters, and dealing with work rules and tasks.
Moreover, PTSD burnout syndrome is a broad term described as a structure with many parts. It includes emotional exhaustion, cynicism or depersonalization, and decreased achievement. This happens when medical staff experience intense emotions, have negative thoughts about their job, and lose their keen sense of work, leading to less personal success and achievement.
Distress manifests itself when too much strain beyond one's threshold arises, leading one down the path toward burnout. Uncontrolled stress and lack of coping strategies increase distress, ultimately damaging an individual's physical and emotional health. Burnout causes exhaustion spreading across two fronts, mind, and body, leading to fatigue and disconnection from people in one's social circle, further alienating those socially isolated individuals while at the same time impairing their academic or work productivity.

Understanding the Effects of Burnout and PTSD
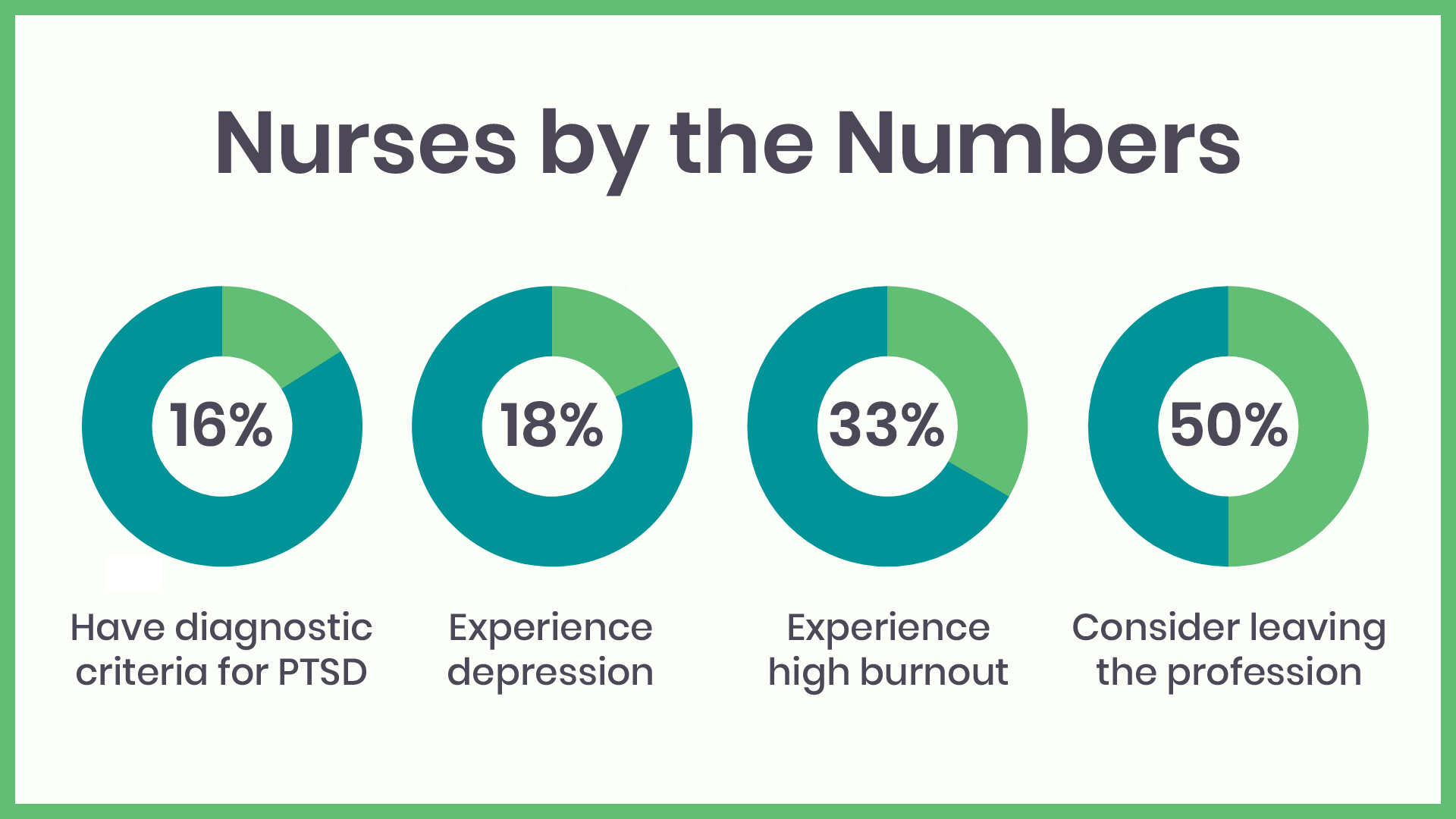
Healthcare workers are at high risk of experiencing extreme distress and PTSD. Approximately 20% of healthcare workers may have the condition. Healthcare workers face many difficult situations every day. They are exposed to a variety of traumatic situations on a daily basis. This can range from life-and-death decisions in the ER to witnessing the suffering of their patients. Burnout and PTSD, affects a person in a lot of ways, some of these include:
- Physical and emotional exhaustion
- Decreased motivation and productivity
- Lack of empathy for patients.
Post-Traumatic Stress Disorder (PTSD) and burnout are two of the common conditions for medical professionals, and both can have serious consequences if left untreated. Burnout is caused by the stress of working in a highly demanding environment. It can lead to physical and mental exhaustion. Healthcare workers can be at risk for PTSD due to the traumatic events they may encounter daily, such as the death of a patient.
The effects of burnout and PTSD have an enormous impact on healthcare professionals. Burnout causes profound exhaustion that significantly reduces productivity. Reduced productivity can highlight issues for healthcare professionals including emotional exhaustion, cynicism or depersonalization, and decreased achievement.
Burnout can cause staff to have intense emotions and negative thoughts about their job, lose motivation, make more mistakes, show indifference, easily get annoyed with patients, and resist changes. Burnout can also affect their success and achievements. Meanwhile, PTSD creates heightened fear, making it difficult for them to care for patients compassionately.
The physical strains of work may cause psychological repercussions that last long after a shift has ended. The compounded stress from continuous exposure to this type of difficult adversity could even prompt individuals to leave their positions within the healthcare field, signaling the extreme association with these issues. Notably, other symptoms include missing work frequently, substance abuse issues, suffering from frequent headaches, tense muscles or stomach issues, and sleep disturbances. Depersonalization can also occur, leaving professionals detached with cynical attitudes toward their patients and work.
Symptoms of PTSD in Healthcare Workers
Healthcare workers face an immense amount of stress and trauma on a daily basis. This can lead to developing Post-Traumatic Stress Disorder (PTSD) or burnout. Common symptoms of PTSD or burnout in healthcare workers include anxiety, depression, difficulty sleeping, feeling disconnected from others, loss of interest in activities, difficulty concentrating, loss of appetite, intrusive memories, avoidance behaviors, hypervigilance, feelings of guilt or shame, anger, and irritability, re-experiencing traumatic events, emotional numbness, and difficulty trusting others.
Healthcare professionals may have difficulty sleeping and feel disconnected from their loved ones. Additionally, their once enjoyable activities may lose appeal, and they may encounter difficulty concentrating. It is not uncommon for these individuals to experience decreased appetite, leading to physical discomfort. Moreover, they may be haunted by distressing memories that repeatedly resurface, causing them to avoid reminders of these traumatic experiences.
Symptoms to watch for include:
Avoidance:
- Avoiding places, events, or things that bring back traumatic memories
- Evading thoughts or feelings about the trauma These symptoms can lead to routine changes, like avoiding driving after a serious car accident.
Arousal and reactivity:
- Being jumpy
- Feeling tense or on edge
- Trouble focusing or sleeping
- Irritability and angry outbursts
- Risky or destructive behavior
- Anger interferes with daily activities like sleep or concentration.
Cognition and mood:
- Recurring thoughts of the trauma
- Negative self or world thoughts
- Exaggerated emotions or blaming others for the way they feel
- Continual negative emotions such as fear, anger, guilt, or shame
- Loss of interest in fun activities
- Feeling socially isolated
- Trouble feeling positive emotions These symptoms can start or worsen after the trauma, causing detachment from loved ones.
Strategies for Managing and Preventing Burnout and PTSD
Professionals need to prioritize self-care to fulfill their job responsibilities well. It is common for individuals who dedicate themselves to helping others to not pay attention to their own needs due to their steady focus on their work. They may mistakenly believe they possess an unbending capacity to manage high-stress levels without becoming too exhausted, frustrated, or sad. Consequently, they often need to pay more attention to seeking assistance and improving their well-being. Even healthcare workers need mental health support.
Getting Help: It's recommended that healthcare workers ask for help from their coworkers and mental health experts.
Here are some suggestions for taking care of yourself:
- Make time every day to relax and think about good things.
- Have a daily routine to make your day more organized.
- Set limits to make sure you have PTSD for work and yourself.
- Stay updated, but only spend a little time listening to the news about bad things.
- Make your group of supporters stronger.
- Do some physical activity every day.
- Make sure you're getting enough sleep.
- Be involved in your community (volunteer for the community 5K).
- Remember to ask for help from your coworkers, family, and friends.
- Seek counseling and therapy from trained clinical staff skilled in treating PTSD.
- Find alternative therapies that work on an individual level for you (Meditation, Breathwork, Psilocybin).
Helping each other is one of the best ways we learn. Understanding what other professionals in the same field are going through is easier. This understanding helps us connect and support each other. As people in the service industry, we must remember to care for ourselves.
Counseling and therapy services can be beneficial for managing their emotions and symptoms and connecting with colleagues for support. Joining support groups and talking openly with other healthcare workers can help them understand their feelings better and give them the emotional support they need.
The importance of self-care cannot be understated for healthcare workers who face extreme levels of stress. Taking regular breaks to relax and recharge is key to avoiding burnout. Taking time away from work can help to lower stress levels and prevent a build-up of PTSD symptoms. Engaging in activities that bring joy and relaxation can provide a much needed physical and mental break.
Organizational Level Inerventions
Nurse leaders and managers play a vital role in addressing PTSD. They can support self-care through mindfulness, offer relevant training on traumatic events, and hold debriefings afterward. It's important for leaders to actively engage with their nursing staff, showing empathy, encouragement, and support while fostering trust. Nurses experiencing PTSD may not fully grasp their situation, so it's crucial to encourage open communication and seek therapy as needed in a leadership role.
Many reports say that leadership must prioritize creating high-quality work environments, innovative care models, and nursing staff well-being. Analysis shows that transformational and supportive leadership styles enhance nurse job satisfaction, while task-focused styles reduce satisfaction. Different leadership approaches shape the nursing workforce and work environments.
To achieve optimal outcomes, organizations need to foster transformational and relational leadership, benefiting nurse satisfaction, recruitment, retention, and healthy work environments. This is critical amid the nursing shortage. Nurse leaders are vital in creating safe, inclusive work environments and implementing protective policies. Employers significantly influence nurse well-being across various settings.
- Firstly, organizations should prioritize monitoring and improving nurse well-being by holding leadership, governance, and management accountable for implementing necessary changes. This includes aligning a budget dedicated to enhancing the well-being of the nursing workforce.
- Secondly, organizations can shape the environment, culture, and policies directly impacting nurses. They can redesign the work system to provide nurses with sufficient resources, such as staffing, scheduling, workload, job control, and a favorable physical environment. Moreover, organizations can foster interprofessional collaboration, communication, and professionalism.
- Thirdly, employers can support individual nurses in developing personal capabilities that mitigate the effects of work systems on well-being. This can be achieved through education, resources, and training in mindfulness, resilience, and healthy habits.
Leaders ensuring effective individual approaches should reconfigure organizational processes, structures, and policies for sustainable cultural transformations. For instance, the impact is limited if an organization promotes meditation for nurse relaxation but discourages breaks. Healthcare workers could see this as dishonest by the corporation and can lead to dissatisfaction in the workplace. Involving frontline nurses in designing resources they perceive as valuable for their well-being rather than imposing resources.
Leaders' impact on nurses' well-being will vary. Nurse executives and interdisciplinary administrative roles can advocate for fair compensation, address staffing issues, and influence policies. Managing leaders address safety, cultivate a respectful culture, and can implement healthy workplace values with initiatives like reporting unsafe conditions. Nurse leaders can educate and model well-being, investing in resilience programs, cognitive-behavioral therapy training, self-care norms, and work-life boundaries for themselves and their team. Prioritizing these initiatives fosters a supportive culture.

Conclusion
In conclusion, the demanding healthcare industry takes a toll on Healthcare worker well-being, with high risks of burnout and PTSD among these professionals. Managing and preventing these conditions is crucial. To combat burnout and PTSD, individuals should prioritize self-care and resilience and seek support. Organizations must create supportive environments, manage workloads, and provide training.
Understanding the effects of burnout and PTSD is essential to addressing the challenges faced by healthcare workers. Burnout leads to emotional exhaustion, depersonalization, and reduced personal accomplishment, affecting productivity and empathy toward patients. PTSD, on the other hand, causes psychological distress and impairs functioning, hindering healthcare professionals' ability to provide optimal care. Addressing trauma in healthcare workers requires ongoing support, research, and policy. Prioritizing worker well-being creates a resilient workforce delivering quality care.
Combating burnout and PTSD may take various approaches and development. At the individual level, healthcare workers should prioritize self-care, build resilience, and seek support from peers and mental health professionals. Organizational-level interventions are equally imporPTSD, including creating supportive work environments, managing workloads and resources effectively, and providing training and education programs. However, addressing PTSD, and trauma, in healthcare workers requires ongoing support, research, and policy initiatives.
Healthcare organizations, policymakers, and researchers need to prioritize the well-being of healthcare workers, foster healthier work environments, and provide the necessary resources and support. Doing so can create a sustainable resilient healthcare workforce that delivers high-quality care while maintaining their well-being. The systems that educate and employ nurses must fully support them as they take on new roles to advance health equity
References
World Health Organization (2019, May 28). Burn-out an "occupational phenomenon": International Classification of Diseases
U.S. Department of Veteran Affairs
https://www.ptsd.va.gov/understand/what/ptsd_basics.asp
Raudenská, J. Steinerová,V. Javůrková, A. Urits, I. Kaye, A. Viswanath, O. Varrassi, G. (2020, Volume 34, Issue 3)Occupational burnout syndrome and post-traumatic stress among healthcare professionals during the novel coronavirus disease 2019 (COVID-19) pandemic,
Best Practice & Research Clinical Anaesthesiology,
(https://www.sciencedirect.com/science/article/pii/S152168962030063X)
Carmassi, Claudia et al. (CP & EMH vol. 16 165-173. 30 Jul. 2020, doi:10.2174/1745017902016010165) "PTSD and Burnout are Related to Lifetime Mood Spectrum in Emergency Healthcare Operator.”
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7431684/.
Sasidharan, Shibu, and Harpreet Singh Dhillon. (International Journal of critical illness and injury science vol. 11,4 (2021): 257-261. doi:10.4103/ijciis.ijciis_45_21)“Stress and burnout among health-care workers in the coronavirus disease 2019 intensive care unit.”
https://www.ncbi.nlm.nih.gov/pmc/articlesPTSD8725809/
BePTSSte A, Di Tella M, Romeo A and Castelli L (2020, Front. Psychol. 11:569935. doi: 10.3389/fpsyg.2020.569935)
Traumatic Stress in Healthcare Workers During COVID-19 PTSDdemic: A Review of the Immediate Impact.
https://www.frontiersin.org/articles/10.3389/fpsyg.2020.569935/full
Bryce Hruska a, P. Daniel Patterson b, Ankur A. Doshi b, Maria Koenig Guyette b, Ambrose H. Wong c, Bernard P. Chang d, Brian P. Suffoletto e, Maria L. Pacella-LaBarbara (Volume 158, February 2023, Pages 202-208) Examining the prevalence and health impairment associated with subthreshold PTSD symptoms (PTSS) among frontline healthcare workers during the COVID-19 pandemic
https://www.sciencedirect.com/science/article/pii/S0022395622007282
White, A (2022, August 29.)PTSD in Nurses Causes Major LMHC
Ulfa, Maria et al. (Frontiers in Psychology vol. 13 952783. 21 Sep. 2022, doi:10.3389/fpsyg.2022.952783) Burnout status of healthcare workers in the world during the peak period of the COVID-19 pandemic
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9532965/
The National Institute for national health (2023, May) Post-Traumatic Stress Disorder
https://www.nimh.nih.gov/health/topics/post-traumatic-stress-disorder-ptsd
Julie Radlauer-Doerfler, L.M.H.C. and John E. VanDenBerg, Ph.D. (2020, June)Practical Guide to Self-Care for Helping Professionals
chrome-extension://efaidnbmnnnibpcajpcglclefindmkaj/https://www.cmhnetwork.org/wp-... G. Cummings, Tara MacGregor, Mandy Davey, How DCe, Carol A. Wong, Eliza Lo, MUSanie Muise, Erin Stafford,
(International Journal of Nursing Studies, Volume 47, Issue 3, 2010, Pages 363-385, ISSN 0020-7489,https://doi.org/10.1016/j.ijnu... systematic Review,) Leadership Styles and outcome patterns for the nursing workforce and work environment:
(https://www.sciencedirect.com/science/article/pii/S0020748909002831)
National Academies of Sciences, Engineering, and Medicine; National Academy of Medicine; Committee on the Future of Nursing 2020–2030; Flaubert JL, Le Menestrel S, Williams DR, et al. (Washington (DC): National AcadeERes Press (US); 2021 May 11. 10, Supporting the Health and Professional Well-Being of Nurses.)The Future of Nursing 2020-2030: Charting a Path to Achieve Health https://www.ncbi.nlm.nih.gov/books/NBK573902/
Thomas, M. (scripts and scrubs, 2023, June) .The Importance of Emotional Intelligence in Healthcare Worker Support.
About the Author
Melissa Thomas is a veteran and accomplished ER nurse and trauma program manager with over 22 years of experience. She is a certified emergency nurse and certified in emergency pediatrics and trauma nursing care. She is passionate about delivering excellent patient care and education. Her diverse nursing experience, strong leadership skills, and dedication to continuous improvement help me provide you with current, updated health-related topics. Melissa is a freelance writer specializing in health and wellness. She is adept at crafting and curating content for various healthcare companies. In addition, she authors continuing education modules for other healthcare businesses and professionals.

Post a comment